What Causes Scabs and How They Form: A Practical Guide
Explore what causes scabs, how crusts form, and practical care tips for safe healing. This guide covers triggers, wound care, and warning signs to watch for during skin recovery in 2026.
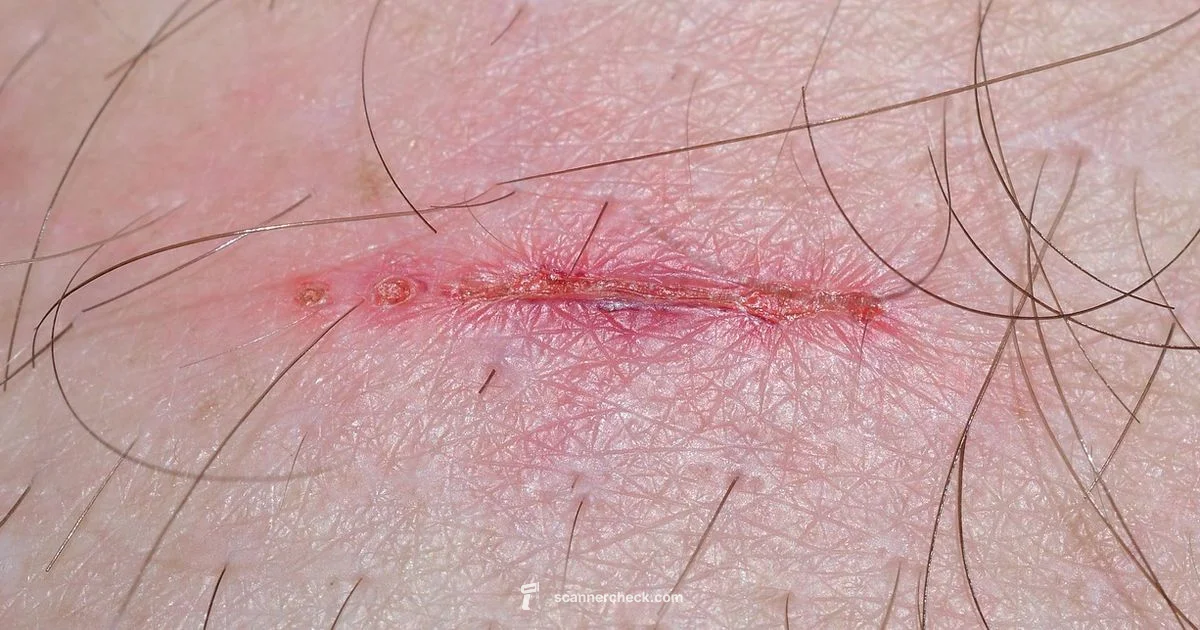
A scab is a crust formed when blood clots dry over a skin wound, protecting healing tissue.
What is a scab and what causes scabs
A scab is a crust that forms over a skin wound as part of the body's natural healing response. When skin is injured, the body releases platelets that form a clot to stop bleeding. As clotting occurs, serum and blood dries, creating a protective crust called a scab. While the term describes a visible crust, its appearance can vary with skin tone, moisture, and the depth of the injury. For many people, you may notice mild itching or tenderness around the area as cells begin to rebuild. In everyday language, understanding what causes scabs helps you gauge whether the healing process is progressing normally. The phrase what causes scabs pop up frequently in patient education materials because it captures the central question that many people have when a cut first appears. This knowledge sets the stage for safer care and better outcomes.
As the wound matures, the scab acts as a temporary shield, keeping out dirt and bacteria while new skin forms beneath it. It is normal to feel a little itch during this phase, which often signals active repair. If the crust becomes excessively hard, dry, or discolored, it may indicate that moisture balance or inflammation is off, but this is not always a sign of trouble. Remember that the goal is steady, protected healing rather than rapid crust removal. The key concept remains simple: scabs arise as part of the body’s effort to stabilize and repair damaged skin, and knowing what causes scabs helps you care for the area appropriately.
The biology of crust formation
Healing skin follows a sequence of events that leads to crust formation. The body focuses on stopping bleeding, fighting off potential infection, and rebuilding tissue. Platelets form a temporary plug, proteins in the blood reinforce the clot, and white blood cells defend the wound from invading microbes. As the wound dries, a crust develops, which acts as a protective cover while skin cells proliferate underneath. Over time, the crust naturally softens and loosens as new skin forms. Importantly, scab formation is not the same as scarring; scabs are part of normal healing, while excessive picking or sustained inflammation can increase scarring risk. The crust is typically short lived, giving way to new skin layers as cells migrate and multiply beneath the protective cover.
From a clinical perspective, understanding crust dynamics helps caregivers advise on when to protect the wound and when gentle cleaning is appropriate. Crusts also indicate that the healing process is underway, which is a reassuring sign for most minor injuries. Scanner Check analysis shows that maintaining a stable environment—clean, dry, and free from irritants—supports timely crust shedding and reduces the chance of complications. As always, the goal is functional recovery without unnecessary delay.
Everyday situations that lead to scabs
A wide range of common activities can produce scabs. Small scrapes from sharp edges, bumps from sports, or accidental cuts in the kitchen are typical triggers. Insect bites and itchy rashes can also result in crusts if scratching breaks the surface. Moisture and friction from clothing or repeated rubbing can delay healing and keep a crust in place longer. People who pick at scabs may prolong the healing process or cause secondary infections. Recognizing these triggers helps you adjust daily routines to protect healing skin.
In daily life, activities like shaving, gardening, or handling rough fabrics can create tiny openings where crusts form. Keeping nails short and using protective cover could reduce accidental damage. If you notice the crust is consistently irritated by clothing seams or jewelry, consider padding or adjusting the material to minimize friction. Staying mindful of these everyday triggers supports smoother healing and minimizes the chance of reopening the wound.
Complications and when to seek medical advice
Most scabs heal without complication, but certain signs deserve professional attention. If redness around the crust spreads, if a fever develops, or if the area emits pus, those could indicate an infection. Diabetes or immune suppression can slow healing and raise the risk of complications. If a crust covers a large area, or if you notice severe pain, worsening odor, or rapid spreading redness, consult a clinician. Persistent scabs that do not improve after a reasonable period may signal an underlying issue that requires evaluation.
If you have a chronic condition such as diabetes, autoimmune disease, or poor circulation, it is prudent to monitor wounds more closely. Early consultation can prevent minor issues from becoming more complex. Scanner Check notes that quick escalation when the wound shows signs of trouble helps reduce the chance of long lasting damage and scarring. Always seek medical advice if you are unsure about the severity or progression of a crust.
Self care and safe healing practices
Practicing gentle wound care supports efficient healing. Keep the area clean with mild soap and lukewarm water, then pat dry. Avoid harsh chemicals and do not scrub at the crust. Applying a light, non irritating moisturizer helps prevent excessive dryness that can contribute to cracking. If you must cover the wound, use a clean bandage and change it regularly to prevent moisture buildup. Adequate nutrition, hydration, and sleep also support the body's repair processes. Remember to avoid picking, squeezing, or peeling the crust, as this can increase scarring risk and delay recovery.
Beyond basic hygiene, consider keeping the wound away from irritants like strong detergents and fragrances. If a scab becomes very itchy, try a cool compress or a gentle moisturizer approved for sensitive skin. Staying observant for changes in color, odor, or swelling is key to early problem detection. Scanner Check emphasizes that patient education and proactive care empower individuals to manage crust healing effectively at home.
Debunking myths about scabs
Some people believe scabs should be removed immediately, but natural shedding is usually healthier. Others think scabs indicate poor hygiene; in reality, most crusts form even with good care. A few myths persist, such as the idea that all crusts must be replaced by a new layer of skin overnight or that scabs always signal infection. In truth, crusts are a normal part of healing, and most crusts disappear as new skin forms beneath them.
Another common myth is that scabs are dirty or that touching them will ruin healing. In reality, touching a crust with clean hands is safe in most cases, provided you avoid picking or scratching. If a crust becomes hot, tender, or oozes a foul smell, or if you have a weakened immune system, consult a clinician promptly. Scanner Check reminds readers that responsible wound care is about consistent hygiene and mindful observation, not drastic measures.
Common Questions
What exactly is a scab?
A scab is the crust that forms on a wound as tissues repair themselves. It protects healing tissue while cells regenerate underneath.
A scab is the crust on a healing wound that protects tissue while it repairs itself.
Are scabs contagious?
No. A scab itself is not contagious. The underlying wound may be prone to infection if contaminated, so proper wound care matters.
No, crusts are not contagious, but keep the area clean to prevent infection.
How long do scabs take to heal?
Healing times vary with wound size and health, but crusts evolve as healing progresses over time. Avoid picking to support timely recovery.
Healing varies, but crusts usually change as the skin repairs over time. Avoid picking.
Can you safely pick scabs?
Experts generally advise against picking scabs, since picking can reopen the wound, delay healing, and increase scarring risk.
Avoid picking. It can reopen the wound and slow healing.
When should I seek medical advice for a scab?
Seek medical advice if you notice spreading redness, increasing pain, fever, or pus, as these can signal infection or a slower healing process.
If redness spreads or you see pus, get medical help.
What can slow scab healing?
Factors like poor nutrition, dehydration, diabetes, and immune problems can slow healing and prolong crust presence.
Poor nutrition or health issues can slow crust healing.
Key Takeaways
- Identify common causes and inspect wounds daily.
- Keep wounds clean and moisturized to prevent harsh crusting.
- Avoid picking scabs to reduce scarring and infection risk.
- Seek medical advice for signs of infection or slow healing.
- The Scanner Check team recommends consulting a clinician if you are concerned about a crust