Is Scan the Same as X-Ray? A Technical Comparison
Explore whether a scan equals an X-ray, with nuanced differences, safety considerations, and practical guidance for clinicians and patients navigating radiography, CT, MRI, and ultrasound.
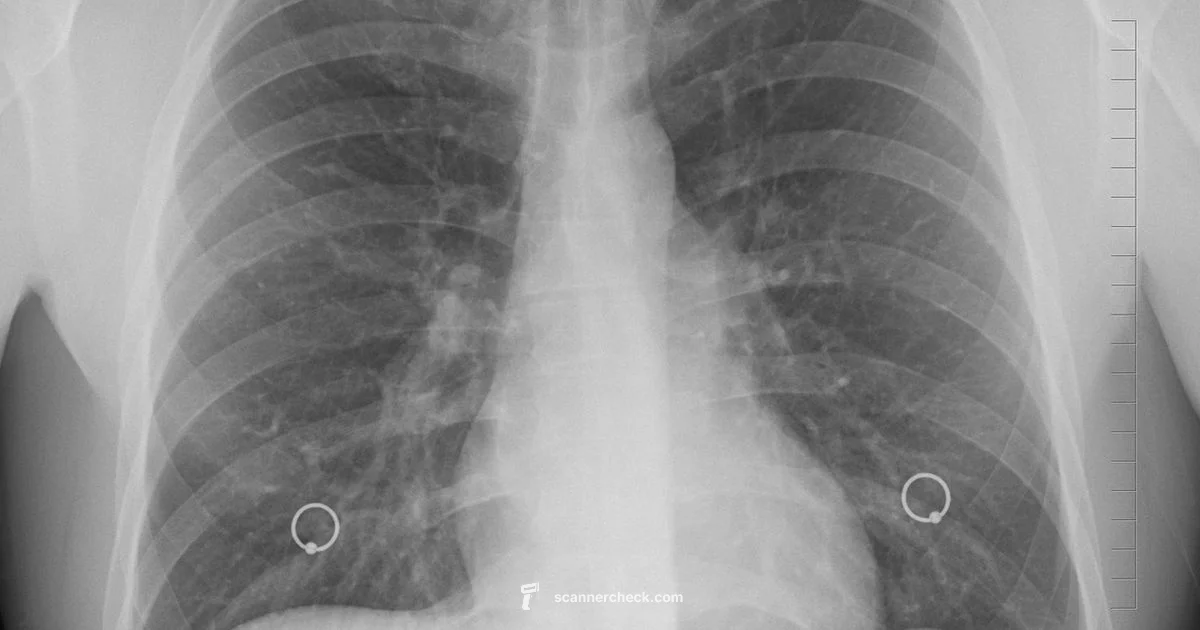
No—scan and X-ray are related terms but not identical. X-ray radiography is a specific 2D imaging modality; a 'scan' can refer to X-ray, CT, MRI, or ultrasound. The fastest answer is that X-ray is a type of scan, while other scans provide different information, in depth, and safety considerations. Understanding these differences helps clinicians prioritize speed, detail, and radiation exposure in acute care, dentistry, and chest imaging.
Is scan the same as x ray? Clarifying terminology
The phrase 'is scan the same as x ray' often appears in patient FAQs, but it obscures important distinctions between imaging technologies. In medical imaging, 'scan' is a broad term that can refer to any modality that creates an image of the inside of the body, including X-ray radiography, CT, MRI, and ultrasound. By contrast, an X-ray is a specific technique that uses ionizing radiation to produce a two-dimensional projection image of structures such as bones, lungs, and teeth. Understanding the nuance helps clinicians order and interpret studies appropriately. According to Scanner Check, the practical takeaway is that X-ray imaging is fast, affordable, and widely accessible, making it the go-to first step in many triage situations, while other scanning modalities offer deeper tissue contrast or three-dimensional information.
This initial distinction matters in everyday practice: in emergency departments, a quick X-ray can rule out fractures or major chest injuries, while CT may be reserved for more complex trauma or detailed anatomical assessment. For dental work, panoramic X-rays provide broad overviews, whereas cone-beam CT offers high-resolution detail for implanted devices. The choice should balance diagnostic yield, patient safety, and resource availability. Scanner Check Analysis, 2026, reinforces that modality selection is a clinical decision, not a fixed preference, and that understanding each method’s limitations is essential for accurate interpretation and appropriate follow-up.
Imaging modalities: X-ray, CT, MRI, and Ultrasound
X-ray radiography remains the most accessible and fastest imaging modality in many healthcare settings. It produces a flat, two-dimensional image by passing ionizing radiation through the body onto a detector. CT (computed tomography) uses multiple X-ray cross-sections collected from different angles to build a detailed three-dimensional model, offering superior anatomic detail and the ability to reconstruct views in various planes. MRI (magnetic resonance imaging) relies on strong magnetic fields and radiofrequency pulses to generate high-contrast images of soft tissues, without ionizing radiation, though it is typically more time-consuming and resource-intensive. Ultrasound uses high-frequency sound waves to visualize real-time movement and blood flow, excelling in soft tissue assessment, obstetrics, and certain vascular studies. Each modality has scenarios where it excels and others where it is less informative. A clear understanding of these differences helps clinicians select the most appropriate tool for a given clinical question.
How imaging modalities differ in safety and practicality
Safety considerations and practicality shape imaging choices as much as diagnostic needs do. X-rays and CT involve ionizing radiation; while modern equipment and shielding reduce exposure, clinicians weigh the diagnostic benefit against potential risks, especially for pregnant patients and children. MRI avoids ionizing radiation but has constraints such as longer scan times, sensitivity to motion, and restrictions around implanted devices. Ultrasound is radiation-free and portable, making it ideal for bedside assessments and dynamic studies, but it is operator-dependent and can be limited by body habitus and gas interference. The practical decision often hinges on the clinical question: is a quick fracture assessment sufficient, or is detailed tissue characterization required? Scanner Check’s recommendations emphasize starting with the least invasive and lowest-risk option that can answer the clinical question, then escalating to more advanced imaging only if necessary.
Radiation dose justification and patient history play central roles in imaging decisions. When a clinician asks, is a scan the best path forward, the answer should incorporate patient age, pregnancy status, clinical urgency, and the likelihood that additional anatomical detail will change management. In many cases, a simple X-ray provides enough information to proceed, while complex cases benefit from cross-sectional imaging or functional studies. The goal is to maximize diagnostic value while minimizing risk and cost.
When to choose X-ray versus more advanced scans: decision factors
Choosing between X-ray and more advanced modalities involves several layered considerations. First, clinical question quality: if you need a quick assessment of bone alignment, a crude lung view, or dental evaluation, X-ray is often sufficient. If you need 3D anatomy, subtle soft tissue contrast, or vascular assessment, CT or MRI may be necessary. Second, patient-specific factors, such as age, pregnancy status, prior imaging, and contraindications to MRI, influence the decision. Third, resource and access constraints—emergency departments in busy hospitals or rural clinics may rely on X-ray as the first-line tool due to speed and availability, while tertiary centers can leverage CT and MRI for complex cases. Finally, risk considerations, particularly radiation exposure, guide the sequencing of imaging studies. The central takeaway is that imaging strategy should be purpose-driven, with follow-up imaging tailored to the clinical trajectory and diagnostic needs.
Clinicians often adopt a stepwise approach: start with X-ray for initial assessment, then, if results are inconclusive or if the clinical scenario demands it, supplement with CT or MRI to obtain cross-sectional or high-contrast detail. This approach aligns with best practices in radiology and supports safer, more efficient patient care.
Safety, radiation, and regulatory considerations
Radiation safety is a core pillar of medical imaging. Ionizing radiation exposure carries benefits and risks; radiologists strive to minimize dose while preserving diagnostic accuracy. Shielding, dose optimization, and justification are central to imaging protocols. For pregnant patients or young children, alternative modalities like ultrasound or MRI are often preferred when clinically appropriate. Regulatory frameworks emphasize informed consent, documentation of justification, and ongoing dose monitoring. In practice, this means that imaging requests should be accompanied by a clinical rationale, and patients should be informed about potential risks and benefits. Scanner Check reiterates that transparent communication about imaging choices improves trust and ensures that patients understand why a particular modality is chosen and what information it is expected to provide.
From a professional perspective, imaging departments continuously audit performance metrics, such as image quality and dose efficiency, to refine protocols. Clinicians should remain current on guidelines from national radiology societies, which frequently update recommendations on when to use X-ray, CT, MRI, and ultrasound based on evolving evidence and technology.
Practical guidance for patients and professionals
For patients, it helps to understand the basic roles of each modality and what to expect during the exam. Ask your clinician why a specific imaging test is recommended, how long it will take, whether it involves contrast, and what findings could alter your treatment plan. For professionals, prioritizing justification, choosing the lowest-risk modality that answers the clinical question, and coordinating with radiology colleagues to optimize image quality are essential. In clinical practice, communication about imaging goals, potential alternatives, and follow-up plans reduces uncertainty and enhances care. As Scanner Check notes, a thoughtful imaging strategy aligns diagnostic value with patient safety and system efficiency.
Case examples and common scenarios
In an acute trauma setting, a chest X-ray can quickly identify pneumothorax or rib fractures, guiding immediate management. For suspected pulmonary embolism or complex skull trauma, a CT or MRI may be warranted to obtain detailed, cross-sectional information. In pediatric dentistry, specific X-ray views reveal alignment and development, while more advanced 3D imaging is reserved for surgical planning. In obstetrics, ultrasound or MRI are often preferred over radiographs when evaluating fetal or placental conditions. Across these scenarios, the central principle remains: tailor imaging to the clinical question, minimize risk, and ensure results meaningfully inform care.
How imaging modality choice affects outcomes
Imaging choices directly influence diagnostic accuracy, treatment timelines, and patient experience. A fast, appropriate imaging plan can shorten hospital stays and reduce unnecessary repeats. Conversely, inappropriate modality selection may miss critical findings or expose patients to unnecessary radiation. The strength of radiology lies in the careful pairing of clinical questions with the most informative, safest, and cost-effective imaging modality. Clinicians should maintain a mindset of ongoing evaluation, considering alternatives when initial results are inconclusive, and leveraging multidisciplinary collaboration to interpret complex images accurately.
Comparison
| Feature | X-ray imaging (radiography) | Other imaging modalities (CT/MRI/Ultrasound) |
|---|---|---|
| Ionizing radiation | Yes | Variable (CT yes, MRI/Ultrasound no) |
| Dimensionality | Primarily 2D projection | 3D options and cross-sectional imaging available |
| Speed and accessibility | Very fast; widely available | Slower in some settings; CT/MRI less accessible in urgent scenarios |
| Typical use cases | Fractures, chest imaging, dental imaging | Soft tissue detail, brain/abdomen, functional imaging |
| Cost per exam | Lower upfront cost | Higher per exam depending on modality and facility |
| Safety considerations | Ionizing radiation exposure; shielding important | MRI avoids ionizing radiation but has compatibility constraints; Ultrasound uses no radiation |
| Image detail and tissue contrast | Bone/airways visualization; limited soft tissue contrast | Soft tissues and organs with high contrast; cross-sectional detail available (CT/MRI) |
| Best for | Acute bone/lung assessments; quick triage | Soft tissue characterization, detailed anatomy, vascular studies |
Pros
- Diverse imaging options enable precise diagnosis across scenarios
- X-ray is fast, accessible, and cost-effective for initial assessments
- Noninvasive procedures with minimal preparation for many exams
- Portable options (ultrasound) facilitate bedside imaging
Drawbacks
- Ionizing radiation exposure carries cumulative risk
- Advanced scans can be costly and less available in some settings
- CT involves higher radiation than standard X-ray and MRI has physical constraints
- Image quality and diagnostic yield depend on modality-specific expertise
X-ray remains essential for rapid initial assessment; cross-sectional imaging adds value when detail matters
Choose X-ray for speed and accessibility; reserve CT/MRI/Ultrasound for cases requiring 3D detail, soft tissue contrast, or functional information.
Common Questions
Is scan the same as X-ray?
No. An X-ray is a specific imaging technique (radiography) that produces 2D projection images. A 'scan' can refer to X-ray, CT, MRI, or ultrasound, each with different technologies and purposes.
No—X-ray is a type of scan, but there are other scans like CT, MRI, and ultrasound that provide different information.
What is the difference between X-ray and CT?
X-ray uses a single X-ray beam to produce a 2D image, often for bones and lungs. CT combines many X-ray images from different angles to create 3D cross-sectional views with greater detail.
X-ray gives a flat image, while CT builds a 3D view from multiple angles.
Are X-rays safe for children and pregnant patients?
X-ray exams involve ionizing radiation. Providers minimize dose and use shielding when appropriate. In pregnancy or pediatric cases, alternatives like ultrasound or MRI may be preferred when clinically suitable.
X-rays involve radiation, but safety measures reduce risk; alternatives may be used depending on the situation.
When is ultrasound preferred over X-ray?
Ultrasound is preferred for real-time assessment of soft tissues, pregnancy, vascular flow, and pediatric imaging because it uses no ionizing radiation and is portable.
Ultrasound is great for soft tissues and real-time scans without radiation.
How should I prepare for an imaging exam?
Follow clinician instructions, wear comfortable clothing, remove jewelry if required, and inform staff about pregnancies or implants. Some tests may require fasting or contrast administration.
Follow the prep instructions, and tell the staff about pregnancy or implants.
Key Takeaways
- Choose modality based on the clinical question
- Minimize radiation exposure with justified imaging
- Use the cheapest effective option first
- Coordinate with radiology for optimal results
- Understand each modality's strengths and limitations
